|
The immunotherapy-chemotherapy regimen induced a higher rate of systemic response (brain metastases, 43% vs. 50%) and 2 years (brain metastases, 35% vs. 12.1 months HR = 0.79 95% CI, 0.65-0.95).Ī higher percentage of patients assigned the immunotherapy-chemotherapy combination remained alive at 1 year (brain metastases, 67% vs. The immunotherapy-chemotherapy combination also extended OS among patients with brain metastases (median, 19.3 months vs. 21%) and 2 years (brain metastases, 19% vs. 5.4 months HR = 0.74 95% CI, 0.62-0.89).Ī higher percentage of patients assigned the immunotherapy-chemotherapy combination achieved systemic PFS at 1 year (brain metastases, 36% vs. Results showed improvements in systemic PFS with the combination regimen among patients with brain metastases (median, 10.6 months vs. Characteristics appeared generally similar between these groups and between treatment arms. This analysis included 101 patients with baseline brain metastases (immunotherapy-chemotherapy, n = 51 chemotherapy alone, n = 50) and 618 without (immunotherapy-chemotherapy, n = 310 chemotherapy alone, n = 308). Researchers observed benefit regardless of PD-L1 expression or histology.Īt World Lung, David Carbone, MD, PhD, director of the James Thoracic Oncology Center at The Ohio State University Comprehensive Cancer Center and Solove Research Institute, presented results of a post-hoc analysis that assessed the efficacy and safety of the regimen based on presence of baseline brain metastases. Treatment continued until disease progression or unacceptable toxicity.Īs Healio previously reported, the study met its primary endpoint, demonstrating superior OS with the nivolumab-ipilimumab regimen in the intention-to-treat population. 
Patients in the control group received up to four cycles of chemotherapy, plus optional pemetrexed maintenance if eligible. Treatment with nivolumab and ipilimumab continued for up to 2 years, or until disease progression or unacceptable toxicity. Patients in the experimental group received the anti-PD-1 antibody nivolumab (Opdivo, Bristol Myers Squibb) dosed at 360 mg every 3 weeks and the anti-CTLA-4 antibody ipilimumab (Yervoy, Bristol Myers Squibb) dosed at 1 mg/kg every 6 weeks combined with two cycles of concomitant chemotherapy. Patients with adequately treated brain metastases who were asymptomatic for at least 2 weeks prior to first treatment were eligible to participate. .jpg)
All patients had ECOG performance status of 0 or 1, with no known sensitizing EGFR or ALK alterations. The randomized, open-label, multicenter CheckMate 9LA trial included 719 patients with stage IV/recurrent NSCLC. 
Treatment options are limited for patients with advanced NSCLC and brain metastases, and these patients may benefit from checkpoint inhibitor therapy, according to study background. Presented at: International Association for the Study of Lung Cancer World Conference on Lung Cancer (virtual meeting) Sept. The findings - presented at International Association for the Study of Lung Cancer World Conference on Lung Cancer - showed nearly three times as many patients assigned the immunotherapy combination survived at least 2 years.ĭata derived from Carbone D, et al. 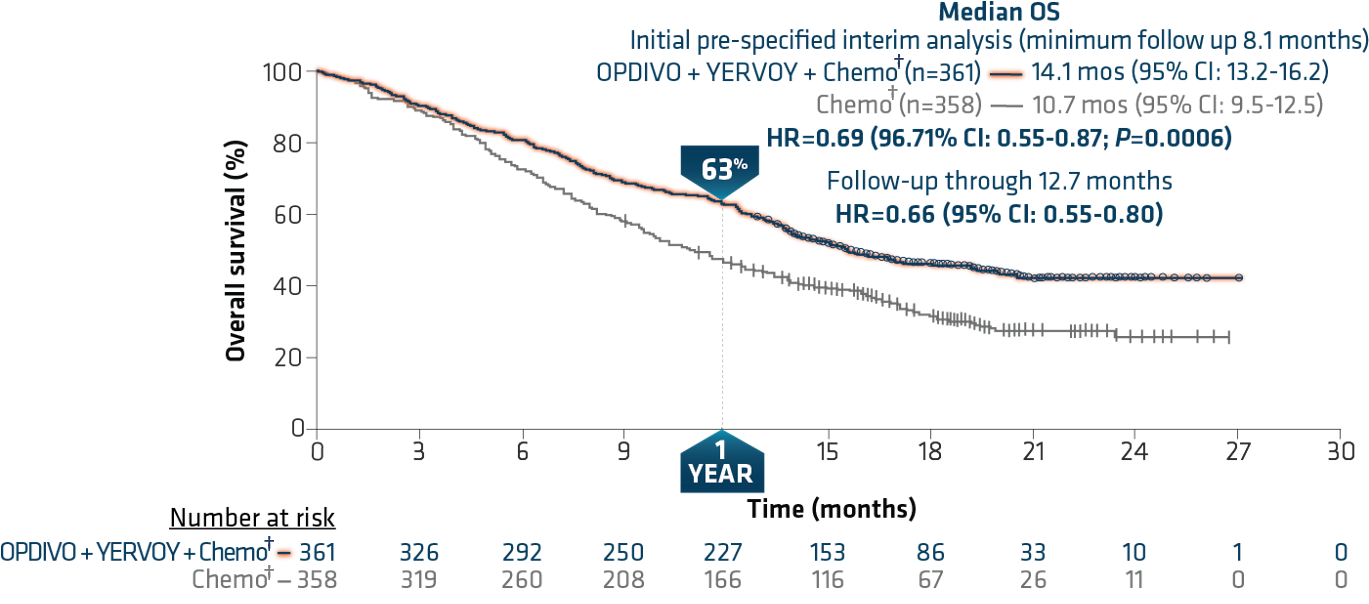
The addition of nivolumab and ipilimumab to first-line chemotherapy conferred durable survival benefits to patients with advanced non-small cell lung cancer and brain metastases, according to results of the phase 3 CheckMate 9LA trial. If you continue to have this issue please contact to Healio
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
